Colitis in dogs
Colitis in dogs is a condition caused by inflammation of the colon. Knowing the characteristic symptoms allows owners to quickly spot health problems and take their pet to a veterinarian for an accurate diagnosis, treatment, and recommendations for proper care.

Content
Causes of pathology
In a dog's body, the large intestine ensures the digestion of nutrients, the absorption of water, and the formation of feces. It can become inflamed due to the following factors:
- Poor diet is one of the most common causes. Excessive consumption of raw vegetables and fruits, fatty or salty foods, low-quality food, and excessively large portions can trigger inflammation.
- External injuries to the abdominal area and internal injuries to the colon due to the ingress of foreign objects (bone fragments, accidentally swallowed toy parts, etc.).
- Infestation with parasites (especially nematodes), whose activity can cause intestinal inflammation and severe pain in the dog.
- Infectious diseases associated with exposure to bacteria, viruses, protozoa (salmonella, clostridia, parvovirus, coronavirus, giardia, trichomonas).
- Food intolerance and allergic reactions (to medications, food). This condition develops as the body's response to a specific protein, high fat content, or the presence of certain additives in food.
- Colon neoplasms (benign and malignant).
- An imbalance of intestinal microflora caused by long-term use of antibiotics.
Symptoms
The main symptom of colitis is a painful, frequent urge to defecate, caused by overstimulation of the colon's receptors. These urges are often ineffective, or the stool produced is small (mixed with blood and mucus), leading dog owners to confuse these conditions with constipation. To relieve constipation, enemas or laxatives are administered, which only worsens the situation.

Characteristic symptoms of the disease also include:
- vomiting (with severe inflammation of the colon walls);
- flatulence;
- bowel disorder;
- belching, rumbling in the intestines;
- lethargy and apathy;
- a sharp decrease in appetite;
- noticeable discomfort when palpating the abdominal area;
- inflammation of the anus;
- exhaustion (anorexia).
Particular attention should be paid to such health problems in pets of breeds most prone to intestinal pathologies. These include: Boxers, Bulldogs (English and French), Shar-Pei, and German Shepherds.
Colitis can occur in dogs in two forms:
- acute – manifested by pronounced symptoms (frequent bowel movements up to 10 times a day, vomiting, lethargy, fever, refusal to eat);
- chronic – there is general weakness of the body due to dehydration, periodic stomach upset and lack of appetite.

The transition of colitis from acute to chronic form is often associated with an incorrect diagnosis in the early stages of the disease or a lack of timely treatment.
Diagnosis and treatment
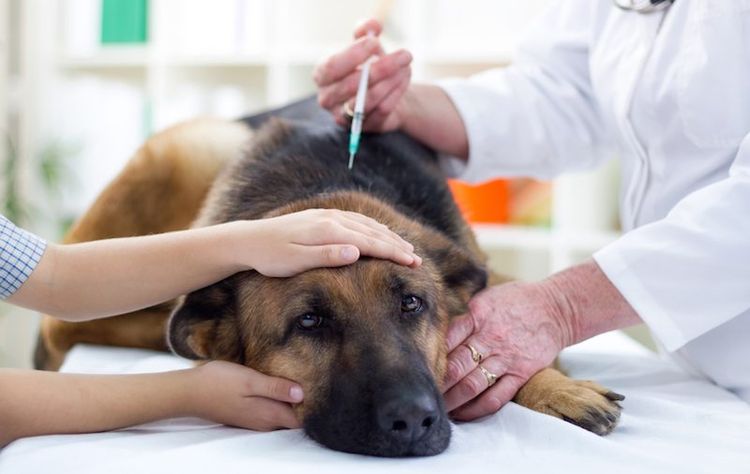
If your pet exhibits any of the above-mentioned symptoms, it's a good idea to take it to a veterinarian for an examination. They will conduct an examination and perform the necessary diagnostic procedures:
- laboratory tests (blood, urine, feces);
- chest and abdominal x-ray;
- Ultrasound diagnostics of the abdominal cavity;
- colon endoscopy.
Treatment will be aimed at:
- elimination of the underlying cause that provoked the pathology;
- restoration of normal intestinal function and its microflora.
Diet
One of the main approaches to treating colitis is a special diet. It is recommended to stop all feedings for the first 24-48 hours until the dog's diarrhea subsides, but ensure adequate water intake. Once the condition improves, you can add the following to the diet:
- chicken, turkey, rabbit meat;
- low-fat dairy products;
- heat-treated vegetables (carrots, turnips),
- a small amount of rice, buckwheat.

During treatment, you should completely exclude from your diet any table food, flour products, canned goods, stewed meat, fatty meat, bones, strong broths, butter, whole milk, and fatty dairy products.
If feeding your dog natural food isn't possible, consult your veterinarian about choosing a therapeutic food to restore the intestinal mucosa and provide the body with essential nutrients. Specialized diets from ProPlan, Hills, and Eukanuba are considered the best for this purpose.
In any case, it's recommended to feed small portions 4-5 times a day. The therapeutic diet usually lasts for about 1-2 months.
Drug therapy
Medications for colitis treatment are selected based on diagnostic results. Depending on the symptoms, the following are prescribed to eliminate the underlying causes of the disease and restore normal bodily function:
- Antibiotics: Kanamycin, Cobactan, Sinulox, Enrofloxacin.
- To relieve diarrhea: Loperamide, Imodium.
- To combat dehydration: Ringer's solutions, glucose, sodium chloride (subcutaneous or intravenous administration);
- To destroy parasites: Furazolidone, Decaris, Piperazine.
- To suppress inflammatory processes: Sulfasalazine, Prednisolone.
- To relieve spasms: No-shpa, Papaverine, Baralgin.
- To restore normal microflora: Colibacterin, Bifidum-bacterin, Linex.
- As adsorbents: Polysorb, Enterosgel.
Typically, therapy can significantly improve a dog's condition within 2-3 days, but a specially formulated long-term diet will help to completely cure the pet and maintain the results. Failure to adhere to the correct diet can result in recurrence of colitis and the need for repeat treatment.
Ignoring the disease can lead to not only severe pain, exhaustion, anemia, and even death for dogs. However, treatment, especially when the underlying cause is identified, typically yields a favorable prognosis. The exception is for animals with cancerous pathologies, where the outcome will depend on the type of cancer cells and their response to therapy.
Preventive measures
The following will help prevent the development of colitis and the subsequent unpleasant consequences associated with it for your dog:
- a balanced diet without adding table food;
- feeding taking into account breed characteristics and weight, without overfeeding;
- prohibition on picking up various objects from the ground during walks;
- choosing safe places for walks;
- timely periodic deworming of the body;
- hygiene control;
- removing from view things that could harm the animal's health (household chemicals, medications, garbage not taken out on time).
Read also:
- Jaundice in a dog after a tick bite
- Ascites in dogs: symptoms and treatment
- My dog is pooping mucus and blood: reasons and what to do
Read also:
- My dog is vomiting yellow or white foam: what should I do?
- Cholecystitis in dogs: symptoms and treatment
- Yellow Vomit in Dogs: Causes and Treatment






5 comments
Natalia
Hello. My puppy is three months old and her only symptoms are blood and mucus, no diarrhea. She's otherwise active, healthy, and has a good appetite. Her temperature is 38°C (it looked like she was in pain when we took it), and she's been dewormed. What could it be?
Dasha is a veterinarian
Hello! What about vaccinations? What's he been feeding? Have you taken him to the vet? Have you had him examined? Not all infectious diseases are accompanied by hyperthermia (an elevated temperature). How long has he been bleeding? Without diarrhea, what is it? Just hard feces with blood and mucus, or loose stools? Is the smell "normal" or sour or otherwise unusual?
Natalia
Hello. She had her booster vaccination on September 3rd (so early because our breeder gave her the first one at 5 weeks). She's been feeding Monge dry food (I've now switched to Proplan). We can't see the vet until the 4th because he's out of town, and we don't have any other vets (it's a small town). She's been bleeding for a week now, and her stools are soft but not runny. I can't comment on the smell because she's always smelly, but I thought it was the dry food.
Dasha is a veterinarian
Hello! Well, then you definitely need to get tested. Without it, a diagnosis can't be made. Is your doctor private? A public clinic never has just one doctor (at least the director, his deputy, and the leading doctors in their departments). Bleeding is abnormal! Try switching to wet food. Ascorutin can sometimes help with bleeding, as can vitamin supplements (look for iron and vitamin K1—they're a must). But you definitely need to see a doctor!!!
Natalia
Thank you.
Add a comment