Signs of rabies in humans after a cat bite
Rabies is an extremely severe and dangerous viral disease caused by the Rabies virus. The primary carriers of the infection are infected wild and domestic animals, including cats. The disease has been known since ancient times and, without treatment, was almost always fatal. Today, medicine has effective treatments, but they must be administered as soon as possible after contact with an infected animal. If a person has already shown signs of rabies after a bite from a cat or other animal, the chances of successful treatment are significantly reduced.

Content
Routes of infection
Wild animals are carriers of the disease. The virus multiplies in their nervous tissue and can be transmitted to another host through saliva. According to the WHO, humans most often become infected with rabies after being bitten by an infected dog. However, transmission by other predators is also common:
- bats;
- foxes;
- skunks;
- raccoons;
- wolves.
Cases rabies in cats Rabies is rare. Pets can become infected through contact with an infected animal, such as while walking outside. Cats living in private homes and allowed to leave the premises without their owner's supervision are at risk of contracting rabies.
The virus enters the body through infected material (saliva) through mucous surfaces or an open wound. This most often occurs during a bite. There is also a risk of infection if the saliva of an infected animal comes into contact with broken skin (with scratches, abrasions, burns, etc.).
Once in the bloodstream, the virus reaches nerve cells in the brain and spinal cord, causing destructive processes. This results in meningoencephalitis, which leads to paralysis of the respiratory system and heart muscle.
The mechanism of infection development
The rabies virus enters the human body through the saliva of an infected animal. The pathogen remains at the site of entry for several hours to a month, where it undergoes primary reproduction (replication).
The virus then spreads along the peripheral nerve fibers to the central nervous system, in particular to the brain, at a rate of approximately 3 mm/hour.
Once in the brain, the virus actively replicates in neurons, causing encephalitis—an inflammation of the brain tissue. Characteristic inclusions known as Babes-Negri bodies form in the affected cells. These specific spherical or oval-shaped granules were first described by scientists Victor Babes and Adelchi Negri.
Babes-Negri bodies play an important role in confirming the diagnosis of rabies during pathological examination of brain tissue.

Signs of rabies in humans
From the moment an infected cat bites until the first symptoms appear, it takes 10 to 50 days. This is the incubation period. During this time, a person may not experience any symptoms, as the virus is only replicating and has not caused significant damage to nerve tissue. During this period, the person can still be saved. However, once symptoms appear, the chances of recovery are virtually zero.
Just 15 years ago, rabies was considered completely incurable once clinical symptoms appeared. But in 2005, the Milwaukee Protocol was first used in the United States, curing a 15-year-old girl. She sought medical attention after symptoms appeared. The disease was successfully treated with an induced coma and high doses of immunostimulants. After 1.5 months, the girl was discharged from the hospital with no signs of rabies. By 2012, five more cases of recovery had been recorded using this method. This suggests that progress in rabies treatment is ongoing, albeit very slowly, and the disease remains deadly.
The clinical picture of the development of pathology in humans is conditionally divided into three stages:
- The prodromal period lasts 1-4 days. The patient experiences general malaise and a slight fever (up to 37.5°C). Severe itching and pain in the wound area, which by this time has long since healed, may be bothering them. Loss of appetite, sleep disturbances, and anxiety may develop.
- Acute phase (1-3 days). The person begins to experience spasms of various muscle groups. Salivation increases, which may manifest as a constant stream of saliva from the mouth and/or the occasional appearance of foam. Aggression, irritability to various external factors (light, sound, odors), and hallucinations occur. Progressive hydrophobia develops, when the person begins to spasm the larynx when attempting to drink water. This pathology is often accompanied by aerophobia – a condition in which spasms and cramps are triggered by even the slightest breeze.
- The paralytic period (1-2 days). The person's behavior becomes less violent as paralysis progresses. Personality manifestations are absent during this stage. Death occurs as a result of cardiac arrest or asphyxia (suffocation).
The duration of the incubation period and the severity of clinical manifestations will depend on the degree of infection by the virus and the state of the person's immune system.

Important! Bites on the hands, face, neck, and genitals are considered the most difficult to treat. These areas contain numerous nerve endings, and the virus will reach its target organs more quickly.
What to do
It is important to remember that rabies treatment will be successful if the victim seeks medical attention immediately after contact with an infected animal, before symptoms appear.
First of all, it is necessary to wash the wound with soap and treat the bite site with ethyl alcohol or another disinfectant solution, since the virus is not resistant to them.
Next, you need to immediately go to the nearest emergency room. You should provide the doctor with all the details of the incident: the animal's behavior, the location of the bite, any scratches, how much time has passed since contact, etc. Based on this information and the patient's condition, the doctor will decide on further treatment.
The primary method of rabies treatment is the administration of the rabies vaccine. The following injection schedule is used: day 0, day 3, day 7, day 14, day 30, day 90. A total of six injections are required. These can be administered in the shoulder or thigh.
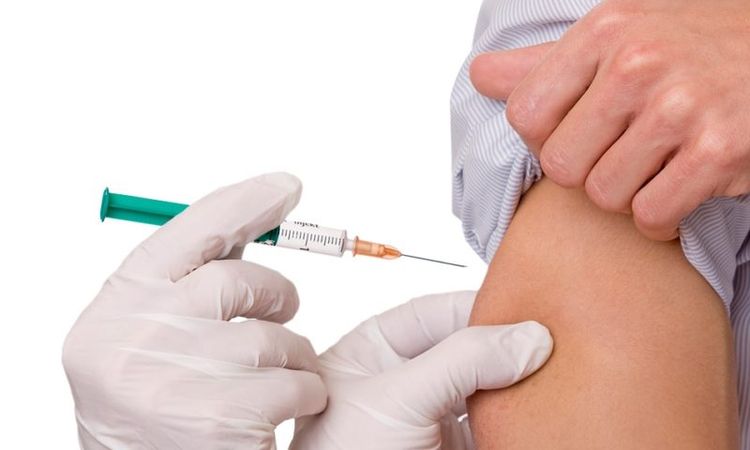
If necessary, anti-rabies immunoglobulin is also used. It is injected into the bite area and surrounding soft tissue. Anti-rabies immunoglobulin may be required for larger wounds or those located near the head.
The vaccination course typically does not require hospitalization. Patients may be hospitalized if they have health problems, severe allergic reactions, or other conditions requiring monitoring (pregnancy, booster vaccination, etc.).
Diagnosis of rabies
It's impossible to accurately determine whether a person has contracted rabies until the first symptoms appear. Anyone who has had contact with an infected or unknown animal is at risk.
After the appearance of signs of the disease, the diagnosis is made on the basis of the characteristic symptoms of rabies: hydrophobia, aerophobia, photophobia, attacks of psychomotor agitation and extensive paralysis.
Laboratory tests serve as an auxiliary diagnostic tool, allowing us to rule out other central nervous system diseases and adjust supportive therapy for a dangerous infectious disease. For this purpose, clinical and biochemical blood tests are performed, as well as electrolyte levels in the patient's body.
Important! The best way to prevent rabies is to vaccinate your pet cats and dogs regularly, especially if they have access to the outdoors.
Read also:
- My cat's hind legs are failing: causes and what to do
- Lump under the skin in cats: what to do
- Taking blood from a cat






Add a comment